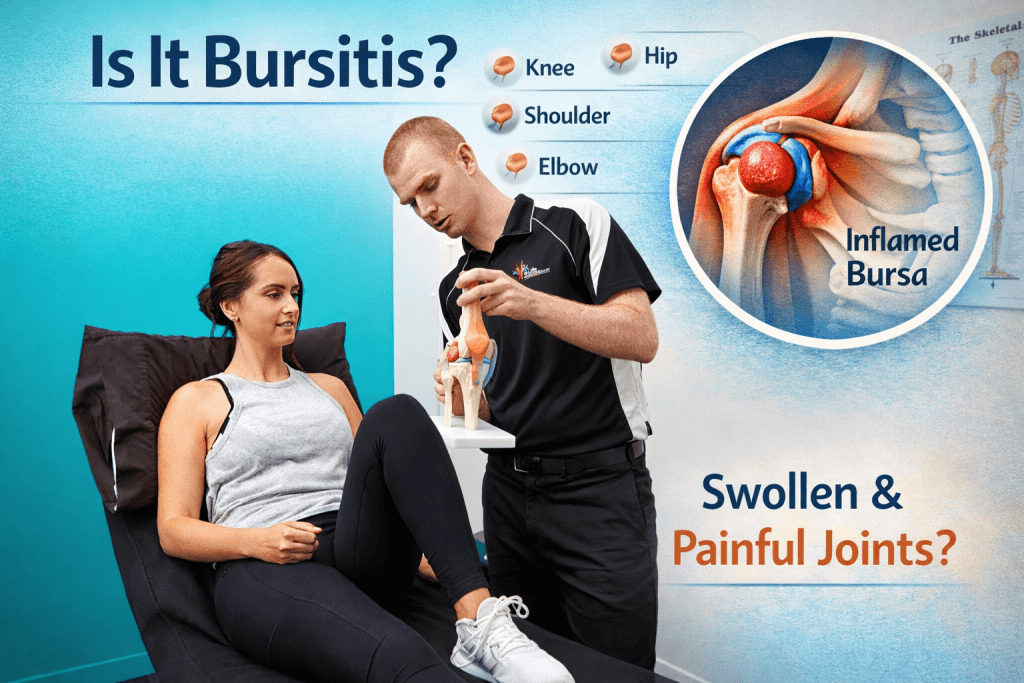
What Is Bursitis?
Think of your joints as having tiny “pillows” called bursae that stop your bones and muscles from rubbing together. When these pillows get irritated or swollen, it’s called bursitis. It makes moving quite painful and stiff, especially in common spots like your shoulders, elbows, hips, knees, or heels.
While a sudden injury can cause bursitis, it’s more often a result of how we move and manage physical “load.” Repetitive motions, poor posture, or staying in one position for too long are common culprits, though medical conditions like diabetes or inflammatory disorders can also play a role. You’ll usually notice it through localised pain and swelling, or a feeling of warmth and stiffness that limits your range of motion.
The good news??
With the right approach, you can achieve a full recovery and get back to the activities you love, pain free. Don’t wait for the pain to linger, seeking a professional assessment early is the best way to prevent the condition from becoming a long-term issue.
Let’s resolve some misconceptions about Bursitis!
Myth 1: “Bursitis is just a sign of aging.”
Fact: While joint changes occur as we age, bursitis is not exclusive to any age group. It is primarily driven by how we use our bodies, through repetitive motion, poor biomechanics, or sudden overload. Whether you are an elite athlete, a manual labourer, or an office worker, anyone can develop bursitis if the physical demands on their joints exceed their capacity to recover.
Myth 2: “Resting will make my bursitis go away”.
Fact: While “active rest” (avoiding specific movements that aggravate the area) is vital during the initial flare up, complete inactivity is counterproductive. Prolonged rest leads to muscle atrophy, joint stiffness, and a lower threshold for physical stress. Without gradual, controlled movement, you risk a cycle of recurring pain the moment you try to return to your normal routine.
Myth 3: “Physiotherapy can’t help Bursitis” or “Exercising makes bursitis worse”.
Fact: Physiotherapy is widely regarded as one of the most effective interventions for bursitis because it treats the root cause, not just the symptoms. Rather than focusing solely on the inflamed bursa, a Physiotherapist analyses movement patterns, muscle imbalances, and workload errors to understand why the area became overloaded. A typical plan includes condition education, lifestyle modifications, and a personalised strengthening program designed to build long term joint resilience.
Myth 4: “My scan showed Bursitis, so it must be my diagnosis”.
Fact: While an Ultrasound or MRI can detect bursal irritation, imaging results don’t always correlate with your level of pain. Many people show signs of bursitis on a scan despite having zero symptoms, while others experience significant pain that doesn’t show up clearly on an image. Because of this, a clinical assessment, which evaluates your strength, posture, and daily activity, is far more reliable than a scan for determining the best path to recovery.
Myth 5: “Bursitis needs injection and surgery”.
Fact: Most cases of acute bursitis do not require invasive treatments. Injections or surgery are reserved for chronic or severe cases that don’t respond to conservative care.
Myth 6: “Bursitis will keep coming back” or “Bursitis is a permanent condition”.
Fact: Bursitis is not automatically chronic. Most patients recover well from bursitis with the right approach. Recurring or persistent bursitis often means that the underlying cause has not been addressed.
Take home message – Bursitis is not just an inflammation; it is a sign of an underlying biomechanical fault that needs to be diagnosed and managed using a Physio guided approach.

By Vinita Rai
Physiotherapist